Coordination capacity as infrastructure
Every complex system has a coordination layer.
Most have never measured theirs.
What AI is revealing
Every complex system runs on two layers most people can see and one layer most people cannot. The visible layers are the work itself and the tools that support it. The invisible layer is the coordination that connects them.
It has never been written into job descriptions. It has never been recorded in datasets. It runs on informal knowledge, personal relationships, and workarounds accumulated over years.
AI is not creating the problem. It is revealing it.
When technology accelerates one layer of a system without the coordination layer scaling with it, the strain becomes visible. Sometimes as tools that get rejected. Sometimes as tools that get adopted and tear the coordination underneath. The same pattern appears across cancer care, across research collaborations, across any high-stakes team operating under cognitive load and specialisation gradient.
The failure gets attributed to personality, culture, or resistance.
The actual cause is a layer that was never specified.
The designer-absorber gap
The people who design the systems are not the people who absorb the demands those systems create. This is true of clinical workflows. It is true of AI implementations. It is true of most technology deployed into complex collaborative work.
The people who absorb the workflow weren't in the room when the decision was made.
In legacy systems, this gap widens invisibly until the system breaks visibly. Successful pilots do not scale because the pilot tested the technology layer and never instrumented the human coordination layer. The next project begins with the same missing input.
This is not a temporary problem. It is a structural gap being encoded into the architecture of the next generation of systems.
The Six Dimensions Framework
Six dimensions of coordination capacity, built from analysis of 69+ peer-reviewed studies on healthcare team coordination across 25+ countries.
Each dimension measurable. Each one actionable.
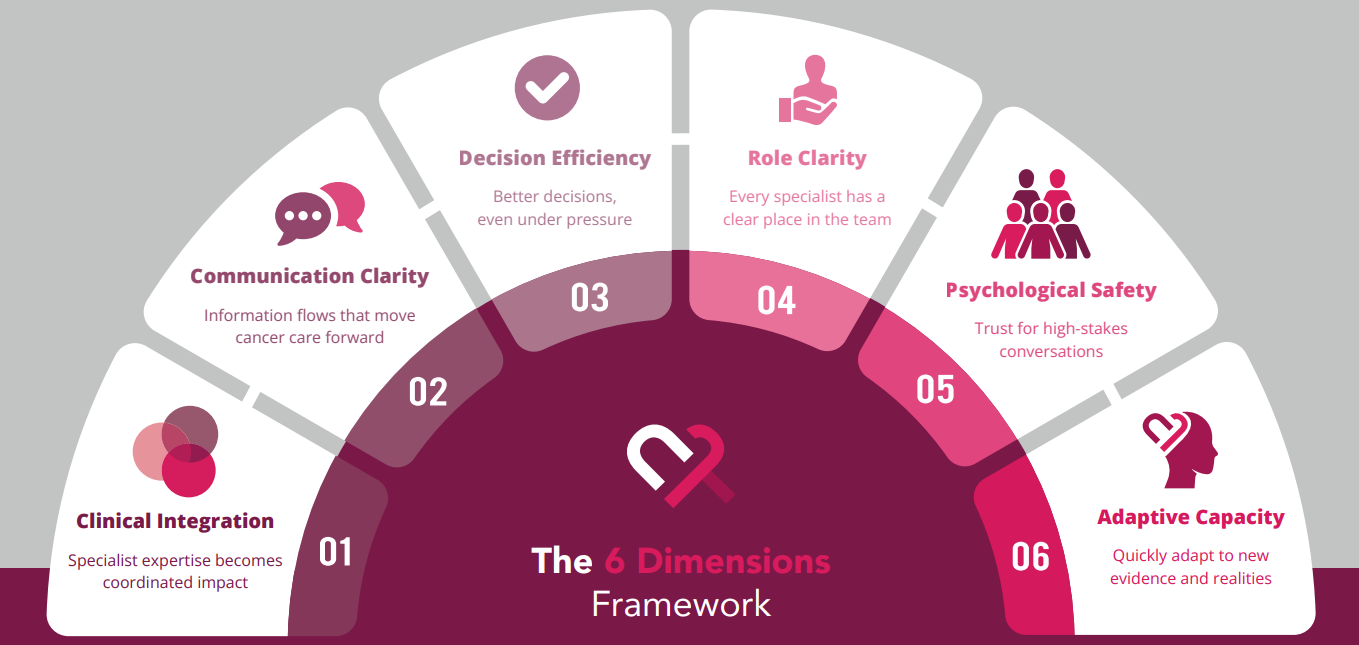



These are the six places where coordination works or breaks in your team. The study measures all of them.
Explore where cancer care coordination works or breaks
The framework was built in cancer care because that is where coordination load is accelerating fastest. Multiple specialists, life-stakes decisions, high information density — the conditions where coordination either holds or breaks are most visible here.
What the evidence is showing
The Cancer Care Coordination Study is the first cross-sectional measurement of coordination capacity across cancer care roles and settings. It is live, with respondents from more than fifteen countries and multiple disciplines. Three patterns are holding across the dataset.
- Invisible work lives in the gap between what people do and what their roles describe. A medical oncologist carries eight coordination tasks without a single one formally recognised. A palliative specialist carries seven. An oncology nurse carries five that have no name in any job description
- Role clarity at handoff points is the root of what looks like decision inefficiency. When nobody is clear who acts on the output and when, the default is waiting for the next meeting. This is particularly visible at the interface between AI-generated output and clinical decision-making
- The people holding coordination together feel least safe doing so. Nurses carry the most coordination work and report the least psychological safety. Physicians report the most safety and the least information flow. The gap between who holds the system together and who feels safe doing so has rarely been measured
The assessment does not change what practitioners know.
It changes what they can see.
Where the framework travels
If coordination capacity can be made visible in cancer care, it can be made visible anywhere the same conditions appear.
The conditions where coordination capacity is worth measuring:
- High cognitive load per decision
- Multiple specialists whose work must integrate
- Real consequences when coordination fails
- A coordination layer currently assumed rather than designed
This describes multidisciplinary clinical teams. It also describes research consortia, AI implementation teams, greenfield healthcare systems being designed from scratch, and any setting where technology is being introduced into collaborative work that was never explicitly coordinated in the first place.
Start with the coordination. The right AI question follows from there.
What becomes possible when coordination is visible
The system designer who can see the coordination layer builds differently. The clinician who can name their coordination work can claim it. The implementation leader who can measure coordination capacity before deployment designs differently than one who cannot.
Coordination becomes something teams can develop, systems can design for, and organisations can resource. The window to name the coordination layer before it gets designed around is open now. Measurement is how the naming becomes durable.
When invisible work gets named, it starts becoming infrastructure rather than personal burden.
If you want to see where your team stands across all six dimensions, the study takes ten minutes.
